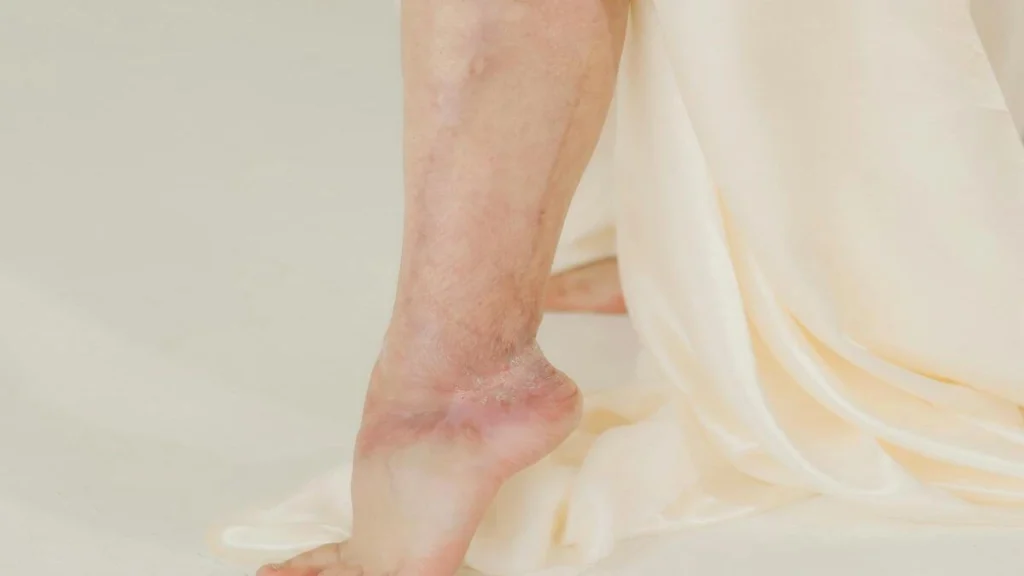
A small cut on the skin usually heals quietly. Within days, inflammation fades, new tissue forms, and the skin closes. However, for millions of people living with diabetes, this simple biological process often goes wrong. Even minor injuries can turn into chronic wounds that persist for weeks or months.
In fact, diabetic foot ulcers are one of the leading causes of hospitalization among people with diabetes. More concerning, they significantly increase the risk of lower-limb amputation.
So why do these wounds refuse to heal?
Traditionally, doctors blamed poor blood circulation and nerve damage. While those factors are certainly important, recent research now highlights another powerful player: the immune system. Scientists are discovering that immune cells inside diabetic wounds behave very differently, preventing the body from completing the healing process.
Understanding this hidden mechanism could transform how diabetic wounds are treated in the future.
First, Understanding How Wounds Normally Heal
To appreciate what goes wrong, it helps to understand how the body normally repairs injured skin.
Wound healing occurs in a series of carefully coordinated stages,
• First comes inflammation, where immune cells rush to the injury site to fight bacteria and clear damaged tissue.
• Next comes the proliferation stage, during which new skin cells multiply and blood vessels begin to grow.
• Finally, the remodeling phase strengthens the new tissue and restores the skin barrier.
Throughout this process, immune cells called macrophages play a critical role. Initially, these cells create inflammation to protect the wound from infection. Then, as healing progresses, they switch into a repair mode that stimulates tissue growth and blood vessel formation.
In healthy individuals, this transition happens smoothly. However, diabetes disrupts this delicate balance.
Meanwhile, Diabetes Keeps the Wound Stuck in Inflammation
One of the most important discoveries in recent research is that diabetic wounds often become trapped in the inflammatory phase.
Instead of switching into repair mode, macrophages remain in a prolonged inflammatory state. As a result, they continue releasing inflammatory chemicals that damage surrounding tissue.
Consequently, the wound environment becomes hostile to healing.
Rather than rebuilding skin, the body remains locked in defense mode. Over time, this chronic inflammation prevents new tissue from forming properly.
This explains why diabetic wounds may appear red, swollen, and slow to close.
In Addition, High Blood Sugar Reprograms Immune Cells
Another critical factor is persistent high blood glucose.
Long term hyperglycemia does not just affect blood vessels. It also alters the internal metabolism of immune cells.
Recent studies show that elevated glucose levels can reprogram macrophages, reducing their ability to promote tissue repair. These cells produce fewer growth factors and healing signals while releasing more inflammatory molecules.
As a result, the wound remains biologically “confused.” The immune system continues fighting a battle that no longer needs to be fought.
Simply put, the body struggles to move from defense to recovery.
At the Same Time, Blood Vessel Damage Slows Tissue Repair
Diabetes also damages small blood vessels in a condition known as microvascular disease.
This damage limits the supply of oxygen and nutrients to injured tissue.
Without adequate oxygen, skin cells divide more slowly and collagen production declines. New blood vessels also struggle to grow, further weakening the healing process.
Therefore, even if immune cells attempt to repair the wound, the surrounding tissue environment may not support proper regeneration.
In many cases, poor circulation and immune dysfunction combine to create a perfect storm for chronic wounds.
Furthermore, Cellular Communication Breaks Down
Healing requires constant communication between different types of cells.
Macrophages send signals that guide fibroblasts, the cells responsible for producing collagen and rebuilding tissue. However, research suggests that this communication becomes disrupted in diabetes.
When macrophages send abnormal signals, fibroblasts may fail to produce enough structural proteins needed for wound closure.
Consequently, tissue repair slows dramatically. You can imagine it like a construction site where the project manager stops coordinating workers. Even if materials are available, progress becomes disorganized and inefficient.
As a Result, Infection Becomes More Likely
Chronic diabetic wounds are also more vulnerable to infection.
High glucose levels provide a favorable environment for bacteria, while weakened immune responses reduce the body’s ability to fight microbes effectively.
Once infection develops, inflammation increases even further. This intensifies tissue damage and slows healing even more.
The wound can become trapped in a cycle of inflammation, infection, and delayed repair.
That is why diabetic foot ulcers require careful medical monitoring.
Encouragingly, Scientists Are Exploring New Treatment Strategies
Despite these challenges, research into diabetic wound healing is advancing rapidly.
Scientists are now investigating therapies that target immune cells directly.
One promising approach focuses on reprogramming macrophages so they switch from inflammatory mode into healing mode. Experimental therapies include advanced biomaterials, immune modulating drugs, and nanotechnology-based treatments designed to restore immune balance.
In addition, researchers are studying exosome-based therapies, which use tiny cellular particles to deliver healing signals to damaged tissue.
Although these treatments are still under investigation, they offer hope for more effective therapies in the future.
Instead of simply treating symptoms, these strategies aim to correct the underlying immune dysfunction.
What Patients with Diabetes Should Know
While new therapies are being developed, prevention remains the most powerful strategy.
Maintaining stable blood glucose levels helps immune cells function more normally and reduces inflammation.
Regular foot care is equally important. Because diabetic neuropathy can reduce sensation, small injuries may go unnoticed.
Therefore, daily foot inspection, proper footwear, and early medical attention are essential for preventing serious complications.
Even a small blister or cut should not be ignored.
The Bigger Picture (A New Understanding of Diabetic Wounds)
For many years, diabetic wounds were viewed mainly as circulation problems.
However, modern research is revealing a more complex story.
Diabetic wounds are increasingly recognized as immune-driven chronic inflammatory conditions. When immune cells fail to transition from inflammation to repair, the healing process stalls.
This discovery is reshaping how scientists approach treatment.
In the future, therapies may not only focus on controlling blood sugar and preventing infection, but also on restoring healthy immune responses within the wound itself.
And sometimes, the most important breakthroughs come from seeing the problem in a completely new way.
FAQs
Q1: Why do wounds heal slowly in people with diabetes?
Wounds heal slowly in diabetes mainly because high blood sugar affects blood circulation, nerve function, and immune responses. As a result, immune cells remain in a prolonged inflammatory state, preventing the body from moving into the tissue repair phase needed for healing.
Q2: What role does the immune system play in diabetic wound healing?
The immune system normally helps clean damaged tissue and then triggers repair. However, in diabetes, immune cells such as macrophages often stay in an inflammatory mode instead of switching to healing mode. This prolonged inflammation delays tissue regeneration.
Q3: Why are diabetic foot ulcers common?
Diabetic neuropathy can reduce sensation in the feet, meaning small cuts or blisters may go unnoticed. At the same time, poor blood flow and immune dysfunction slow healing, allowing minor injuries to develop into ulcers.
Q4: Can high blood sugar directly affect wound healing?
Yes, persistently elevated glucose levels can damage blood vessels, reduce oxygen delivery, and alter immune cell metabolism. These changes disrupt normal wound repair processes.
Q5: Are diabetic wounds more prone to infection?
Yes, High glucose levels create an environment where bacteria can grow more easily. In addition, immune defenses may be weaker, increasing the risk of infection and further delaying healing.
Q6: What new treatments are scientists studying for diabetic wounds?
Researchers are exploring therapies that target immune cells, particularly macrophages, to help them shift from inflammation to repair. Other emerging approaches include regenerative medicine, biomaterials, and exosome-based therapies that support tissue regeneration.
Q7: How can people with diabetes reduce the risk of chronic wounds?
Maintaining stable blood sugar levels, performing regular foot checks, wearing protective footwear, and seeking early medical care for any skin injury are important steps to prevent complications.
Disclaimer
This article is intended for educational and informational purposes only. It does not replace professional medical advice, diagnosis, or treatment. Individuals with diabetes or chronic wounds should consult a qualified healthcare professional for personalized care.
Call to Action
If you found this article helpful, consider sharing it with others who live with diabetes. Raising awareness about proper wound care and early treatment can help prevent serious complications and improve long-term health outcomes.
References
• International Immunopharmacology, Research on macrophage behavior in diabetic wound healing.
• Journal of Tissue Engineering and Regenerative Medicine, Studies on immune cell regulation in chronic wounds.
• Journal of Nanobiotechnology. Research exploring immune-targeted therapies for diabetic wounds.
• European Journal of Medical Research, Review describing chronic inflammation and immune dysfunction in diabetic ulcers.
• National Institutes of Health (NIH), Research highlighting impaired immune response in diabetic wound healing.